Laparoscopic Gastric Banding
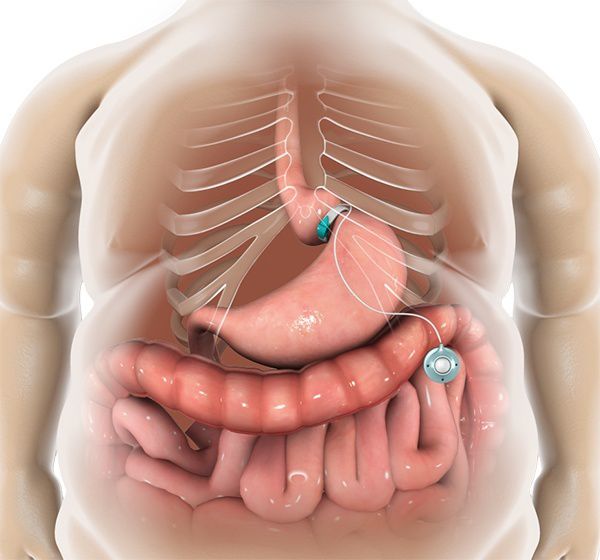
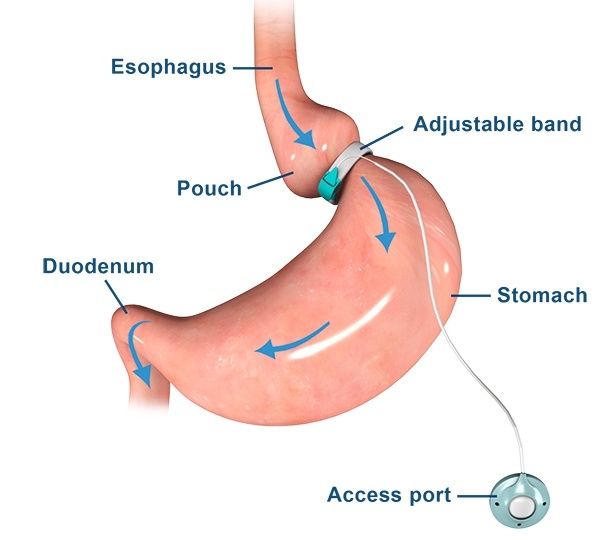
In this procedure, a hollow band made of special material is placed around the stomach near its upper end, creating a small upper stomach pouch and a narrow passage into the larger remainder of the stomach. The band is then inflated with a salt solution. It can be tightened or loosened over time to change the size of the passage by increasing or decreasing the amount of salt solution. The entire procedure is done laparoscopically, where a laparoscope is inserted through the abdominal wall through small surgical incisions.
It induces weight loss by reducing the capacity of the stomach, which restricts the amount of food that can be consumed and slowing down your eating.
Minimally Invasive Approach
During the procedure, surgeons usually use laparoscopic techniques (using small incisions and long-shafted instruments) to implant an inflatable silicone band into the patient’s abdomen. Like a wristwatch, the band is fastened around the upper stomach to create a new, tiny stomach pouch that limits and controls the amount of food you eat. It also creates a small outlet that slows the emptying process into the stomach and the intestine. As a result, patients experience an early sensation of fullness and are satisfied with smaller amounts of food. In turn, this results in weight loss.
This is considered as a day surgery procedure:
- 30 minutes operative time
- Return to work after 2 days
The success of this surgery depends on your commitment and follow-up with your doctor. If lifestyle changes are made and maintained, the benefits of bariatric surgery include:
- Weight reduction
- Improvement in obesity-related conditions
- Improved movement and stamina
- Enhanced mood, self-esteem and quality of life
Least traumatic procedure
Since there is no cutting, stapling or stomach re-routing involved in the laparoscopic gastric banding procedure, it is considered the least traumatic of all weight loss surgeries. The laparoscopic approach to the surgery also offers the advantages of reduced post-operative pain, shortened hospital stay and quicker recovery. If for any reason the gastric band needs to be removed, the stomach generally returns to its original form.
Adjustable treatment
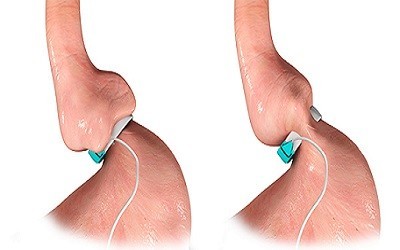
The adjustable gastric banding surgery is an adjustable weight loss surgery. The diameter of the band is adjustable for a customized weight-loss rate. Your individual needs can change as you lose weight.
To modify the size of the band, its inner surface can be inflated or deflated with a saline solution. The band is connected by tubing it to an access port, which is placed well below the skin during surgery. After the operation, the surgeon can control the amount of saline in the band by entering the port with a fine needle through the skin.
Adjustable gastric banding surgery advantages:
Minimal trauma
- Least invasive surgical option
- No intestinal re-routing
- No cutting or stapling of the stomach wall or bowel
- Reduced patient pain, hospital length-of-stay and recovery period
Fewer risks and side effects
- Significantly lower mortality risk than other obesity surgery procedures
- Low risk of nutritional deficiencies associated with gastric bypass
- Reduced risk of hair loss
- No “dumping syndrome” related to dietary intake restrictions
Adjustable
- Allows individualized degree of restriction for ideal, long-term weight loss. Adjustments performed without additional surgery
- Supports pregnancy by allowing stomach outlet size to be opened for increased nutritional needs
Reversible
- Removable at any time
- Stomach and other anatomy are generally restored to their original forms and functions
Effective long-term weight loss
- Typical weight loss 50-60% EWL over two years
Disadvantages
- Band may leak, slip or erode into stomach wall and need removal
- Some foods such as steak and dry chicken will be difficult to eat
- Still easy to cheat: If you choose to drink high calorie liquids or eat chocolate you won’t lose weight!
- If the band is removed or fails, weight regain is nearly always experienced back to preop levels
- Approximately 3-4 % of bands cumulatively/year are being removed, so in 10 years, 30-40% of bands would have been repaired, revised or removed.
- Quality of eating is not as good as for sleeve
What to expect prior to the procedure
Each bariatric surgery program has specific requirements. You may have the following done:
- Thorough physical exam and review of your medical history
- Mental health evaluation and counseling
- Ongoing consultations with a registered dietitian
- Program to help you lose weight through diet and exercise
Leading up to your procedure
- Talk to your doctor about your medications, herbs and dietary supplements. You may be asked to stop taking some medications up to one week before the procedure, like anti-inflammatory drugs, blood thinners and antiplatelets.
- Do not start any new medications, herbs or supplements without talking to your doctor.
- Arrange for a ride to and from the hospital. Also, arrange for help at home.
- If advised by your doctor, take antibiotics.
- The night before, eat a light meal. Do not eat or drink anything after midnight unless told otherwise by your doctor. You may be given laxatives and/or enema to clear your bowels.
- Shower or bathe the morning of your surgery.
Anesthesia
General anesthesia will be used. You will be asleep for the surgery.
Description of the procedure
To prepare you for surgery, an IV will be placed. You may receive fluids and medications through the IV during the procedure. A breathing tube will be placed through your mouth and into your windpipe. This will help you breathe during surgery. You will also have a catheter placed in your bladder to drain urine. Several small incisions will be made in the abdomen. Gas will be pumped in to inflate your abdomen. This will make it easier for the doctor to see. A laparoscope and surgical tools will be inserted through the incisions. A laparoscope is a thin, lighted tool with a tiny camera. It sends images of your abdominal cavity to a monitor in the operating room. Your doctor will operate while viewing the area on this monitor. An adjustable round band is placed around the top of the stomach and fastened into place. This creates a smaller stomach area for food. Tubing is placed from the band to an access port in the abdominal wall. The band can later be adjusted with a special saline solution and needle syringe. The incisions will be closed with staples or stitches.
Immediately after the procedure
The breathing tube will be removed. You will be taken to the recovery area while the anesthesia wears off.
How long will it take?
30-60 minutes.
How much will it hurt?
Anesthesia will prevent pain during surgery. Pain and discomfort after the procedure can be managed with medications.
Post-procedure care at the hospital
While you are recovering at the hospital:
- Pain medication will be given as needed.
- On the day after the surgery, X-rays will be taken to make sure the band is in place. If everything looks fine, you will be given fluids, and can then progress to pureed food.
You may be asked to do the following:
- Use an incentive spirometer to take deep breaths every hour. This is to prevent breathing problems.
- Wear elastic surgical stockings or boots. This is to promote blood flow in your legs.
- Get up and walk to circulate blood and promote healing.
Preventing infection
During your stay, the hospital staff will take steps to reduce your chance of infection, such as:
- Washing their hands
- Wearing gloves or masks
- Keeping your incisions covered
At home
Be sure to follow your doctor’s instructions. You will need to practice lifelong healthy eating and exercise habits. Keep the following in mind after your surgery:
- Do not drive or lift anything heavy until your doctor tells you it is safe. This may take two weeks or more.
- Walk as soon as you are able. Exercise lightly every day.
- Meet regularly with your healthcare team for monitoring and support.
- Ask your doctor when it is safe to shower, bathe or soak in water.
- Follow your doctor’s instructions on driving limitations.
- Your doctor may recommend that you meet with a therapist to discuss emotional changes after surgery.
Your new stomach pouch will be the size of a small egg. It will be slow to empty. This will make you feel full quickly. Nutritional guidelines include:
- Eat very small amounts and eat very slowly. You will begin with 4-6 small meals per day. A meal is two ounces of food.
- For the first 4-6 weeks, all food must be pureed. After you move to solid foods, food must be well-chewed. When making food choices, ensure that you are getting enough proteins.
- Eating too much or too quickly can cause vomiting or intense pain under your breastbone. Most people quickly learn how much food they can eat.
- This procedure does not cause nausea and diarrhea if sweet or fatty foods are eaten. In fact, some people gain back weight because they continue to eat high-calorie foods. To promote ongoing weight loss, you will need to eat healthy foods.
Follow your doctor’s instructions.
You may need to take medications, as directed by your doctor, which may include:
- Medications to reduce stomach acid
- Pain medication such as acetaminophen
- Vitamin and mineral supplements
Ask your doctor if you are able to take medication in pill form. You may need to crush your medication or switch to liquid forms.
Call your doctor
Call your doctor if any of these occur:
- Signs of infection, including fever and chills
- Redness, swelling, increasing pain, excessive bleeding, or discharge from the incision sites
- Pain that you cannot control with the medications you have been given
- Blood in stools
- Constipation that lasts more than two days
- Pain, burning, urgency or frequency of urination, or persistent bleeding in the urine
- Persistent nausea and/or vomiting
- Pain and/or swelling in your feet,calves or legs
- Persistent cough
- New or worsening symptoms
Call for emergency medical services right away for:
- Shortness of breath
- Chest pain